
MEDICATIONS
Medications play a crucial role in comprehensive COPD management in conjunction with healthy lifestyle habits to improve symptoms, improve quality of life, slow disease progression and reduce the risk of exacerbations and premature death.
Appropriate medication use should provide adequate control of breathlessness and flare-up frequency, and improve physical performance. Costs, side effects, and your preferences and abilities to use certain devices are also considered. Therefore, each person’s medication regime is individualised to them and often looks different from one person to another in COPD.
Prescription of medications follow a step-wise approach, and the effects are usually assessed over six weeks before making changes. Medications can be referred to by their generic name (e.g. Salbutamol) or brand name (e.g. Ventolin). Each will have its own potential side effects however, only a small number of people will experience these and your doctor will only prescribe a medication if the benefits outweigh the likelihood of detrimental effects. Medications can be delivered through a range of devices. Devices can also deliver a combination of different medications together. This field is constantly and rapidly evolving, hence it is important to have regular medication reviews with your medical practitioner so that you have the most updated combination for your needs.
To get the most out of your medication regime, know the following for each medication you have been prescribed:

What is it for?

How does it work and how long does it last?

How do you take it?

What are the potential side effects?

When do you need to replenish it?
The information below describes 5 key areas of pharmacological treatment for COPD: inhaler use, oral steroids, long-term antibiotics, oxygen therapy, and vaccinations. Palliative treatments can also be considered for symptoms that remain difficult to control despite optimised standard care.
Inhaled medications
Many medications in COPD are taken via an inhaler device to be delivered directly to the lung airways where they act. Inhalers can be classified as short or long-acting relievers (bronchodilators), or inhaled corticosteroids. (‘Broncho’ = breathing tube, ‘dilator’ = to open) Relievers open up the airways in your lungs by relaxing the muscle bands around them. This improves the flow of air in and out of your lungs during breathing. Relievers either provide quick relief (short-acting), or work gradually over a longer period of time (long-acting).
Short-acting relievers (SABA, SAMA)
- SABA stands for short-acting beta2-agonist.
- SAMA stands for short-acting muscarinic antagonist.
These are often prescribed as a ‘rescue’ medication to provide quick (< 1 minute), short-term relief of symptoms.
General side effects: fast heartbeat, tremors, nervousness, dry mouth, headache.
Long-acting relievers (LABA, LAMA)
- LABA stands for long-acting beta2-agonist.
- LAMA stands for long-acting muscarinic antagonist.
These affect the nerves controlling the muscles around breathing tubes to prevent them from constricting. They should be used regularly, even when you are not feeling symptomatic to enable daily control of symptoms. These medications have been shown to reduce the frequency of flare-ups and hospitalisations, and improve overall quality of life.
General side effects: dry mouth or irritated throat, tremors, dizziness, upset stomach, cardiovascular symptoms such as rapid or irregular heart rate.
Inhaled corticosteroids (ICS)
Breathing tubes can be narrowed by swelling and mucus due to ongoing inflammation in COPD. Corticosteroids are not to be confused with anabolic steroids used to boost muscle bulk and athletic performance, but these work to reduce the inflammation in the inner lining of your breathing tubes and subsequently open them up to improve airflow. Inhaled corticosteroids are often preferred to corticosteroids taken orally because the drug acts more directly on the airways, a smaller dose is required to achieve desired effect, and side effects are lessened.
General side effects: Voice hoarseness and sore throat are the most frequent side effects experienced. These can be minimised with the use of a spacer and mouth rinsing after using your inhaler. Evidence suggests an increased risk of pneumonia associated with long-term use of ICS, therefore the trade-off between benefit and harm is regularly reviewed by your lung specialist.
Combination therapies
Different combinations of inhaled medications are commonly combined into single devices to save you time and make them easier to use. These are represented in the chart below as abbreviations such as ICS/LABA, LAMA/LABA or even ICS/LAMA/LABA.
Many lung health organisations produce detailed charts showing pictures of inhaled medications used to treat COPD. An example from Lung Foundation Australia is available HERE.
– Inhaler devices
Different medications are delivered via different inhaler devices. Certain device types may suit your individual needs and abilities better than others, and some medications are available in different (or comparable) devices. Your doctor or pharmacist is best placed to discuss the right options available for you. The main types of inhalers used in COPD include:

Pressurised metered-dose inhalers
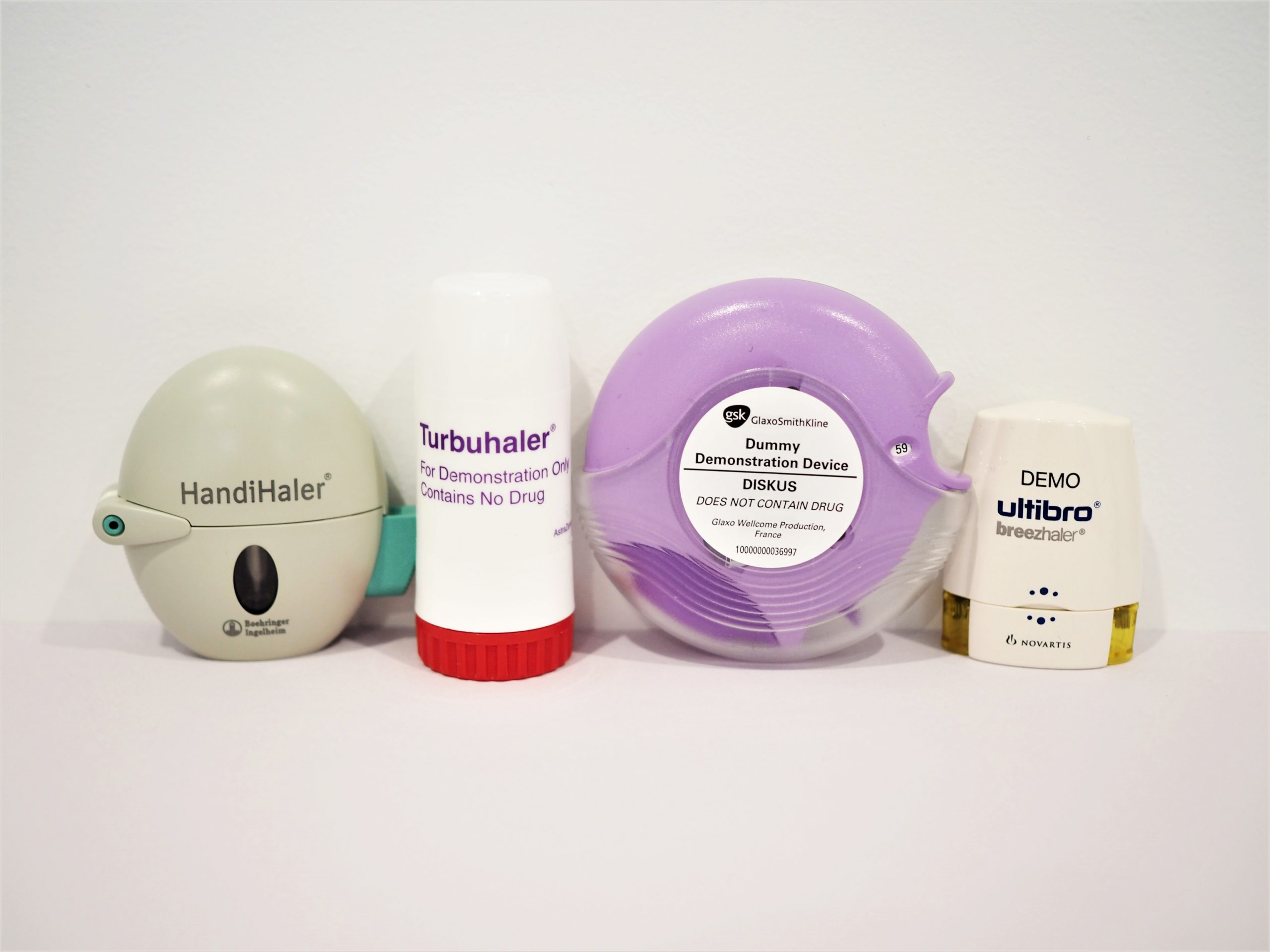
Dry power inhalers

Soft mist inhalers
Learn how to keep your inhalers clean.
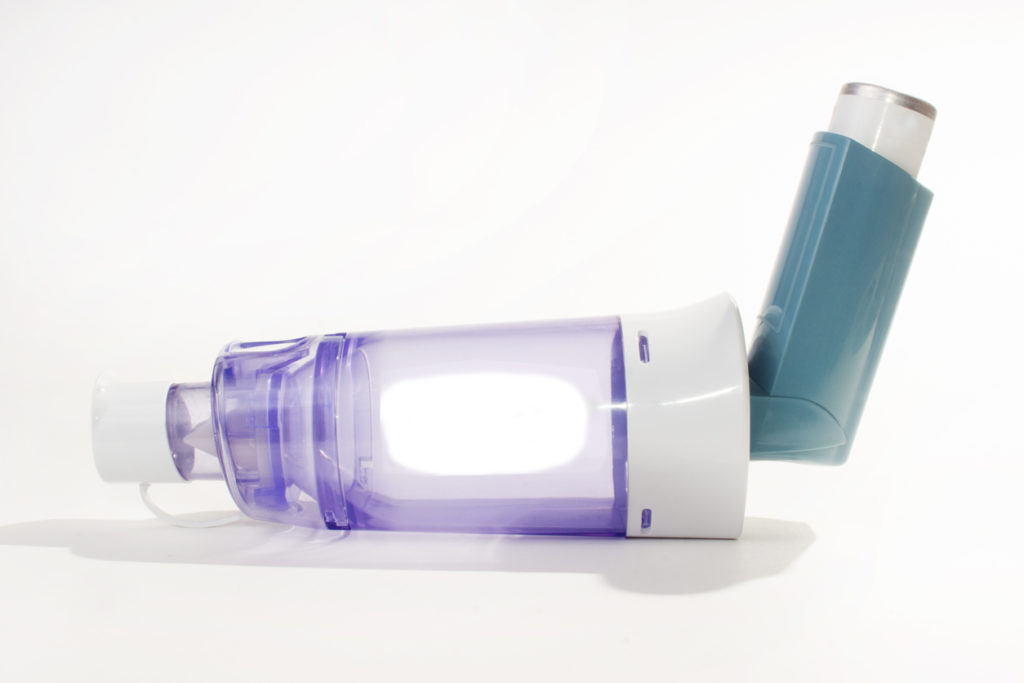
– Spacers
A spacer makes it easier to take medicine from metered dose inhalers and requires less coordination of timing your breathing with pressing the inhaler. Less medication is deposited in your mouth or throat which avoids irritation or infections such as thrush, and this means more medication travels to your lungs. Your healthcare professional can help identify the most suitable spacer for you. Spacers should be cleaned once a month, or after recovering from a respiratory infection (including colds).
More information about spacers including a video demonstration is available via the Lung Foundation Australia website.
– Inhaler technique
Each inhaler type requires a different breathing technique to ensure optimal drug delivery to your lungs for maximum health benefits. Unfortunately, many people use their devices incorrectly. This can be due to poor timing of the inward breath, weak strength of inhalation, or even failure to correctly activate the drug.
Up to 90% of people with COPD do not use their inhaler correctly. Ensure your technique is reviewed by a healthcare professional.
It is crucial that you know how to correctly use your prescribed device(s). Excellent video demonstrations for a range of inhaler devices are available via various lung health societies such as the ones listed below:
Oral steroids
Some individuals may respond favourably on lung function testing or physical function performance to corticosteroids taken orally rather than inhaled. Long-term use of these systemic (system-wide) drugs is not recommended due to the potential for harmful effects, therefore they are generally prescribed over monitored short courses.
Long-term antibiotics
Continuous or intermittent use of antibiotics can be effective in reducing the number of flare-ups for a select group of individuals who suffer these frequently, and improve their quality of life. These individuals are typically 65 years or older, and have moderate to severe COPD. The use of long-term prophylactic (preventive) antibiotic therapy should be discussed with your lung specialist to weigh up potential benefits versus developing antibiotic resistance and harmful side effects.
Oxygen therapy
Oxygen therapy is prescribed for people with COPD whose lungs are not able to keep a sufficient amount of oxygen in their bloodstream for the rest of the body’s cells over a prolonged period of time. This results in damage to vital organs. Doctors will assess this with a blood test, and if the test shows that oxygen saturation levels are adequate, then oxygen therapy is not likely to benefit you. Conversely, long-term (supplementary) oxygen therapy has shown survival benefits for qualifying individuals with stable disease.
If you meet the criteria for requiring oxygen therapy, your doctor will tell you how much supplementary oxygen you are to have each day. Some individuals might only require supplementary oxygen when exerting such as showering or exercising, or only when sleeping. Under usage will not achieve maximal benefits and may continue to expose your vital organs to the consequences of having insufficient oxygen. Overuse can also lead to other medical complications, most commonly respiratory failure.
Find more information about oxygen therapy equipment and safety in the home.
Vaccinations
Individuals with COPD are more susceptible to getting chest infections because their immune systems are less robust, and their lungs have greater difficulty combating irritants. In addition to practicing good hygiene habits and maintaining a healthy lifestyle of diet, sleep and exercise, vaccinations are a key component of avoiding respiratory infections and subsequent unwanted health outcomes.
The annual influenza immunisation lowers the risk of influenza and influenza-like illness in people aged 65 years and older. The pneumococcal vaccination is effective in preventing community-acquired pneumococcal pneumonia. There is a significant additive benefit of receiving dual immunisations in COPD including reduced risks of severe lung complications, flare-ups, hospitalisations and premature death. Discuss any questions you may have regarding your vaccination schedule with your medical practitioner.