
PULMONARY REHABILITATION
Pulmonary rehabilitation (PR) is a structured program consisting of exercise as a cornerstone feature, education about chronic lung disease and self-management, nutritional counselling and intervention, psychological and social support, and smoking cessation assistance. The graphic below depicts the various intervention components of PR which allows the program to be tailored to meet each individual’s needs.
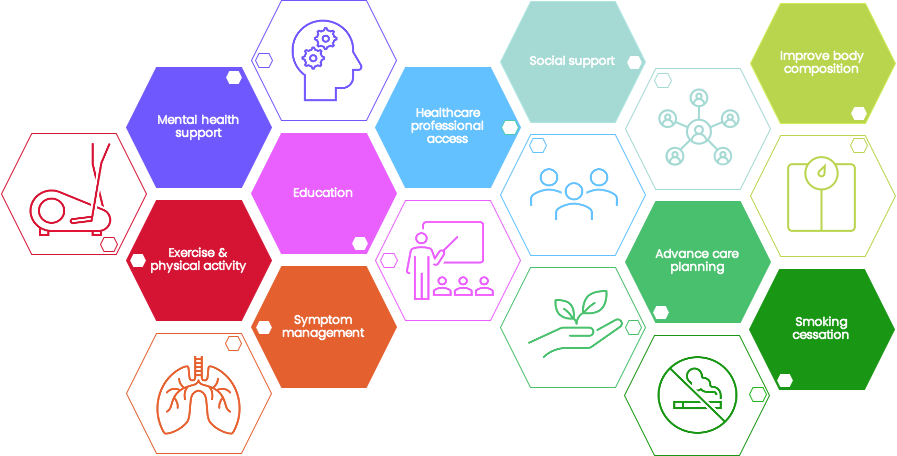
It is the the coordinated bundle of tailored interventions and the intensity of the program that underpin the benefits gained from completing PR. Pulmonary rehabilitation is provided by a team of health practitioners involving doctors, nurses, physiotherapists and other allied health professionals such as dieticians, psychologists or exercise physiologists. More information about PR can also be learnt through Lung Foundation Australia.
Comprehensive information for healthcare professionals regarding the design and delivery of PR programs can be found at the Pulmonary Rehabilitation Toolkit.
Pulmonary rehabilitation is tailored to your preferences, goals and abilities following a comprehensive baseline assessment.
The overall aims of PR are to:
- Reduce the burden of symptoms
- Improve your quality of life
- Reduce the risk of hospital admissions
- Optimise the person’s mental and emotional wellbeing
- Enhance fitness and nutritional status
- Empower the individual for behaviour change
- Improve the person’s ability to cope with flare-up and stable stages of the disease
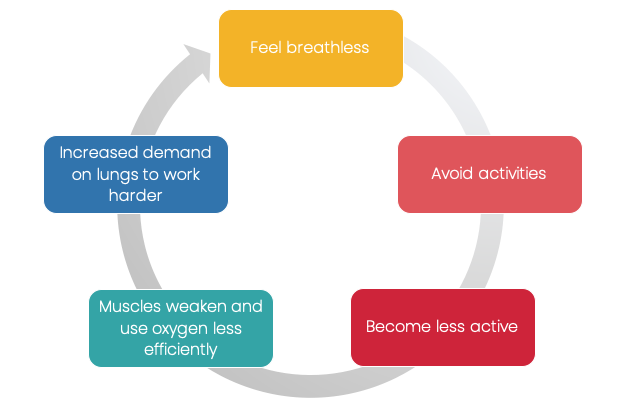
PR helps break and reverse the progressive cycle of inactivity, deconditioning and increased symptoms such as breathlessness and fatigue.
Program structure
Duration: The length of a PR program can vary from country to country, but often runs between 4-12 weeks, attending at least twice per week. In Australia, typical PR is 8 weeks, twice per week. In other countries it can be 12 weeks 3 times per week, followed by 12 weeks twice per week.
Supervision: Most PR programs are supervised by a qualified healthcare professional with expertise in exercise testing and prescription. This is typically a physiotherapist but may also be an exercise physiologist, nurse or other adequately trained professional.
What to expect: The first session is usually focused on getting to know the status of your health and psychosocial well-being through a range of assessments. These typically include interviews by the program’s doctor and nurse and an exercise test like a walking activity to provide baseline information for further exercise prescription in the program. The team then collaborates with you to make further arrangements for other health professionals to be involved in your rehabilitation program based on needs arising from these assessments, and your rehabilitation goals.
Interim sessions will be focused on intervention mainly comprising exercise therapy, and education presentations and discussions with fellow rehabilitation participants. Re-assessments will be completed at the end of the program to measure your progress and determine how to address ongoing needs and goals.
Setting
Pulmonary rehabilitation is traditionally delivered in a healthcare setting such as a hospital outpatient department or community rehabilitation or health centre. In recent years, the rehabilitation landscape has evolved to include alternative models of delivery such as home-based rehabilitation (with varied degrees of supervision), remotely supervised rehabilitation (or ‘tele-rehabilitation’) and online self-paced rehabilitation. More information regarding these models is described here.
Supporting Evidence
Research does support pulmonary rehabilitation to be an effective treatment for many people with bronchiectasis. Some of the reported benefits include:
- Improved ability to exercise
- Reduced breathlessness and fatigue
- Improved quality of life
- Fewer flare-ups
- Improved mental health
Topics that people with bronchiectasis are keen to learn about are:
- What bronchiectasis is, its causes and what is its prognosis
- Self-management (including of acute flare-ups of their lung condition)
- Information about the role of diet and optimising sleep
- The importance of airway clearance therapy, including the options for treatment (and how this may be adapted)
- The role of physical therapy, particularly outside of a pulmonary rehabilitation program
- Treatment for extra-pulmonary conditions, including management of psychological symptoms of anxiety and depression, and the associated stigma of their condition
Most people are happy to receive this information in a group setting, as it enables them to feel a connection with their peers and gain support.
Pulmonary rehabilitation after a lung flare-up
While you are in hospital, a healthcare professional such as your physiotherapist or doctor may talk about referring you to pulmonary rehabilitation after discharge. This may depend on your current level of activity and what you were able to do (or already doing) prior to your flare-up, as some people with bronchiectasis may already have an established exercise routine. If you have not done much exercise in the past, the idea of an exercise program may be daunting. Talk to your healthcare team regarding the options for exercise upon discharge to determine what will be best for you.